AtherosclerosisHardening of the Arteries, Arteriosclerotic Disease, Endarteritis Deformans, Arteriosclerotic Obliterans, Occlusive Arteriosclerosis, Senile Arteriosclerosis
|
Basic Information
What is Atherosclerosis?
Atherosclerosis and arteriosclerosis are degenerative processes that affect arteries throughout the body. The two processes commonly accompany each other. The two terms are often used interchangeably but they differ.
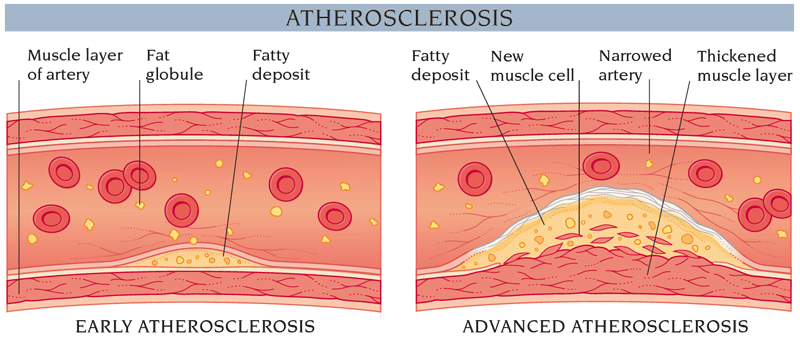
Atherosclerosis is a patchy accumulation of fatty deposits called atheromas or plaques in the walls of large and medium sized arteries. As the atheromas slowly increase in size over the years, they result in areas of narrowing (stenosis). Eventually the stenosis may become severe enough to obstruct blood flow.
Arteriosclerosis (hardening of the arteries) is a diffuse degeneration and calcification of the arterial walls that occurs in arteries of all sizes. It results in loss of flexibility of the arteries.
Atherosclerosis and arteriosclerosis can cause recognizable diseases when they affect the coronary arteries, the arteries to the brain, to the legs, or the aorta. Arteries supplying other organs such as the intestines or kidneys may also be affected but are much less commonly involved.
Risk factors for arteriosclerosis and atherosclerosis include male gender, increasing age, family history of early atherosclerotic disease before age 50, hypertension, diabetes, smoking, high blood cholesterol, obesity, and poor physical fitness. If an individual has multiple risk factors, the risk increases accordingly. Overall, males are at higher risk than females are. The risk increases for females who do not take estrogen after menopause or who have had both ovaries surgically removed (bilateral oophorectomy).
Atherosclerosis signs and symptoms
- Symptoms often are absent until atherosclerosis reaches advanced stages. Symptoms depend on what part of the body has a decreased blood flow and the extent of disease.
- Muscle cramps if atherosclerosis involves vessels in the legs.
- Angina pectoris or heart attack if it involves blood vessels to the heart.
- Stroke or transient ischemic attack if it involves vessels to the neck and brain.
Causes
Patches of fatty tissue, composed of low density lipoprotein that damage artery walls often collect at artery junctions. This collection may begin in early adulthood. At these points, the inner lining of the artery may trap fatty substances that circulate in the blood. As fatty deposits accumulate, they reduce the blood vessel's elasticity and narrow the passageway, interfering with blood flow. They can also crack or tear and form clots that block off the artery.
Risk increases with
- High blood pressure.
- High cholesterol levels (high levels of the low density lipoprotein and low levels of the high density lipoprotein).
- Adults over 60.
- Male sex.
- Stress.
- Diabetes mellitus.
- Obesity; sedentary lifestyle.
- Smoking.
- Poor nutrition (too much fat and cholesterol in the diet).
- Family history of atherosclerosis.
Preventive measures
- Don't smoke.
- Follow suggestions under Diet. Children and young adults of parents with this condition may benefit from a low-fat diet.
- Exercise regularly.
- Reduce stress to a manageable level when possible.
- If you have diabetes or high blood pressure, adhere strictly to your treatment program.
Expected outcomes
Asymptomatic disease usually does not result in disability. However, symptoms may eventually develop, depending on the extent to which risk factors can be modified. In symptomatic disease, the prognosis depends on the specific diagnosis such as coronary, cerebrovascular, or peripheral vascular disease, or aortic aneurysm, the severity and extent of disease, the type of treatment, response to treatment, the presence or absence of complications, and the modification of risk factors.
Possible complications
- Heart attack.
- Stroke.
- Angina pectoris.
- Kidney disease.
- Congestive heart failure.
- Heartbeat irregularity problems.
- Sudden death.
Atherosclerosis treatment
General measures
- Diagnostic tests may include laboratory studies, ECG (electrocardiograph that measures electrical activity of the heart), exercise-tolerance test, blood studies of cholesterol and highdensity lipoproteins, blood sugar tests, and X-rays of the chest and blood vessels.
- Treatment for atherosclerosis is generally directed at its complications.
- Counseling to learn to cope with stress is sometimes helpful.
- Stop smoking.
- Surgical treatment is available in some high-risk patients. Balloon angioplasty can open narrowed vessels; vein graft bypass can help restore blood to the heart; large arterial obstructions can be removed by endarterectomy; entire segments of diseased vessels can be replaced by woven plastic tube grafts.
Medications
- Since the damage has already been done, there is no satisfactory medicine that can treat atherosclerosis.
- Recent studies show that lowering cholesterol levels in persons with high levels can increase life expectancy. If you have symptoms of a disorder caused by atherosclerosis and diet and exercise fail to reduce cholesterol, antihyperlipidemic drugs may be prescribed.
- Other drugs may be necessary to treat symptoms of an associated problem (high blood pressure, heartbeat irregularities).
- Some studies have indicated that aspirin and vitamin E may reduce the risk of heart attack. Get medical advice to see if they should be recommended for you.
| Information | Brand | Generic | Label | Rating |
 |
Lipitor | Atorvastatin |  |
|
 |
Plavix | Clopidogrel |  |
Tenormin (Atenolol), Mevacor (Lovastatin), Pravachol (Pravastatin), Zocor (Simvastatin), Trental (Pentoxifylline)
Activity
- Usually no restrictions. Activity will depend on general state of health and any other illnesses present.
- A routine exercise program is encouraged.
Diet
Eat a diet that is low in fat and low in salt and high in fiber. Increase your intake of grains, fresh fruits and vegetables.
Appropriate specialists
Internist, cardiologist, cardiovascular surgeon, neurologist, and vascular surgeon.
Notify your physician if
You or a family member has high risk factors for atherosclerosis and want to become involved in a prevention program.
Last updated 20 May 2015
